Translate this page into:
Coping Styles and Life Satisfaction in Palliative Care
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Background:
Patients in palliative care suffer variously due to underassessment of needs and suboptimal intervention, coupled with lack of access to palliative care. This study attempts to identify effective coping strategies which lead to life satisfaction, among those afflicted with terminal cancer.
Materials and Methods:
This observational, cross-sectional study was carried out among terminally-ill cancer patients undergoing palliative care. Cancer patients receiving palliative care who give consent and were aged 18 years or older were included in the study. Those with cognitive deficits, delirium, or psychosis were excluded from the study. COPE scale, Temporal Satisfaction with Life Scale, and sociodemographic Performa were administered and analyzed. Pearson's r correlation coefficient test and multiple linear regression analyses were used to evaluate correlation and effect of coping strategies on life satisfaction.
Results:
Religious coping was the most frequently used coping strategy by patients, followed by acceptance. Females showed higher problem-focused coping, whereas males had higher emotion-focused and avoidant coping strategies. Females manifested more religious coping. Males showed more acceptance of their illness. Those without a partner had significantly higher emotion-focused coping strategies and higher religious coping. Income, social support, and problem-oriented coping were positively related to quality of life. Life satisfaction showed significant negative correlation with denial, substance use, and venting utilized as coping methods.
Conclusion:
Problem-focused coping (religious coping and acceptance) was found to be more effective than other methods. Patients in palliative care could be instructed for the use of problem-focused coping. Such training might enhance their life satisfaction, helping them experience greater control over the course of illness.
Keywords
Coping
life satisfaction
palliative care
quality of life
INTRODUCTION
Palliative care began with a focus on the care of the dying. Dr. Cicely Saunders first articulated her ideas about modern hospice care in the late 1950s based on the careful observation of dying patients. She advocated that only an interdisciplinary team could relieve the “total pain” of a dying person in the context of his or her family. Palliative care patients suffer unnecessarily, owing to widespread underassessment and suboptimal treatment of their problems and lack of access to palliative care.[1] Too little intervention is also common in the form of poor pain control, malnutrition, dehydration, and lack of emotional and social support.[234]
Over the past 20 years, prevalence of advanced cancer and increased life span has been a reality. It is estimated that one million new cases of cancer occur each year in India, of which over 80% present at Stages III and IV.[5] There will be a sizeable population of the aged who will have several spells of hospitalization interspersed with long periods of being confined to their beds at home.[6] Patients living with chronic/terminal illnesses have various associated stressors, for example, major decisions about health, treatment-related issues, changes in social relation, anxiety about future and death dependency on others, limited physical functioning, service-related stressors, stress related to adherence to treatment, and side effects.[7]
Stressors of chronically-ill patients also include concerns about the lives of their family members, well-being of significant others along with patients' need to have good social relations, wanting to live longer with their partners, concern for the welfare of their younger children and that they would no longer be available to bring up their kids, guilt for considering themselves accountable for their disease and for causing distress in their children's lives, concerns regarding the method of disease disclosure to their children, coping with the effect of their illness on their family members, and concern over social suffering and personal pain due to their perception of falling short of their life responsibilities.[89]
Coping is the process of using emotional, cognitive, and/or behavioral strategies to manage one's stress in order to reduce its potential harmful impact on psychological adjustment as shown in Figure 1. Coping styles are associated with psychological distress in a number of different populations.[1011] Problem-focused coping is negatively associated with stress, anxiety, and depressive symptoms, while avoidant coping is positively associated with stress, anxiety, and depression. The research surrounding emotion-focused coping has produced mixed findings, with some studies showing it to be associated with increased distress and others decreased distress. This appears to occur because emotion-focused coping encompasses a broad range of coping strategies, each with varying effectiveness.[12]
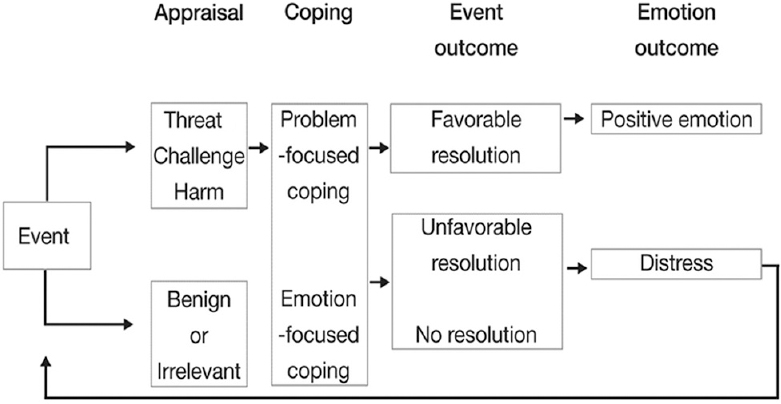
- Theoretical model of the coping process
Having effective coping mechanisms may be one of the most important predictors of well-being across the life span. The aim of this study is to explore the relationship between coping strategies and satisfaction with life (SWL) of patients in palliative care patients.[131415] The present study shall try to identify the effective coping strategies, which leads to SWL, even if one is afflicted with a chronic disease, such as cancer or HIV.
Aim and objectives
-
To assess the coping strategies among patients under palliative care
-
To study the correlation between coping strategy and SWL among terminally ill patients.
MATERIALS AND METHODS
A structured interview schedule was conducted including COPE scale, Temporal Satisfaction with Life Scale (TSWLS) scale, and sociodemographic pro forma. Demographic and medical characteristics were analyzed using descriptive statistics. Pearson's r correlation coefficient test was used to determine whether there is a relationship between specific coping strategies and SWL among the study population. Subsequently, multiple linear regression analysis was done examining the effect of coping strategies on TSWLS scores. An independent t-test and ANOVA test analysis were used to determine an association between demographics and coping strategies.
Inclusion criteria
-
Cancer patients receiving palliative care
-
HIV-AIDS patients receiving palliative care
-
Patients who give consent
-
Aged 18 years or older
-
Had been diagnosed with incurable cancer in the past 6 months.
Exclusion criteria
-
Those who did not give the consent
-
Patients with cognitive deficits, delirium, psychosis.
Instrument
The COPE inventory consists of sixty items, which were divided into 15 subscales having four items in each scale. These subscales were positive reinterpretation and growth, active coping, planning, seeking social support for emotional reasons, seeking social support for instrumental reasons, suppression of competing activities, religion, acceptance, mental disengagement, behavioral disengagement, focus on and venting of emotions, restraint coping, alcohol and drug use, and humor.[16]
TSWLS: This scale was developed by Pavot et al. It contains 15 items which were related with past, present, and future SWL. The scoring ranges from (1) strongly disagree to (7) strongly agree. All items were positively worded. The retest reliability (4-week interval) was 0.83 and alpha reliability was 0.92 (Pavot et al., 1998). The retest reliability (8-week interval of Hindi version was 0.77 (Dubey and Agarwal, 2004; Dubey, 2003). The Hindi version of this scale was significantly correlated with (r = 0.79) the original English version.[17]
DISCUSSION
Among the total participants, the patients' ages ranged from the youngest at 28 to the oldest at 70 years (mean = 46.15, standard deviation [SD] = 8.72). A total of 58 patients were staying with their partner, whereas 42 patients did not have partner support either due to divorce/separation or death. A total of 42 patients were educated at least till primary education, whereas 52 patients were uneducated. There were no significant differences in occupation and education between the groups of patients. Majority of the patients were employed (56%). About 43% of patients were those who were recently diagnosed under the palliative care category (time since diagnosis <1 year).
Females had significantly higher mean scores of problem-focused coping strategies compared to males (P = 0.04), whereas males had higher emotion-focused and avoidant coping strategies (P < 0.05). Females had higher mean of religious coping compared to males. Males had more acceptance of their illness than females.
Older age people had significantly higher mean scores of problem-focused coping strategies compared to younger age group (P = 0.04).
People living without a partner had significantly higher mean scores of emotion-focused coping strategies compared to those staying with a family member (P < 0.001). Patients living alone had higher mean of religious coping and lower mean scores of acceptance and humor compared to other group (P = 0.01).
Educated patients had significantly higher mean scores of emotion-focused coping strategies compared to uneducated patients (P = 0.038). Educated patients had higher mean of acceptance and lower mean scores of avoidant coping compared to other groups (P < 0.05). Employed patients had significantly lower mean scores of emotion-focused coping strategies compared to unemployed patients (P = 0.038). The differences between all other coping strategies was nonsignificant.
Duration of illness <1 year had significantly higher mean scores of avoidant coping strategies compared to patients with longer duration of illness (P = 0.038). Longer duration of illness had higher mean of problem-focused coping, humor, and religious coping compared to other group (P < 0.05).
This chart shows that the most common coping strategy used by the patients was religious coping, followed by use of emotional support and the least common was substance use as shown in Table 1.

Religious coping was the most frequently used coping strategy by patients. Acceptance was the second most frequently used coping strategy of patients as shown in Table 2. The three strategies that were commonly used by the patients were both emotion focused and problem focused as shown in Figure 2. It may be concluded that patients use both types of strategies to combat the stress. Income, emotional social support, and problem-oriented and perception-oriented coping were positively related to quality of life (QOL). Significant negative correlation between SWL and denial and substance use and venting was also found in the current study. The total SWL has lower mean in the study participants (mean = 49.11, SD = 12.72) compared to the general population (mean = 63.61, SD = 16.03).


- Coping strategies in study patients
The total SWL was overall higher among the cancer patients (mean = 51.05, SD = 13.12) compared to HIV patients (mean = 46.20, SD = 11.68). Patients had lowest score of present SWL with mean of 15.65 and 13.40 among cancer patients and HIV patients, respectively. On the temporal scale, the patients had highest SWL in the past with mean of 19.20 and 17.35 among cancer patients and HIV patients, respectively as shown in Table 3.

The results showed that coping strategies of patients namely humor and religion were positively related to their total SWL (r = 0.58, P < 0.01 and r = 0.22, P < 0.05, respectively). For the coping dimension, problem-focused coping was positively related, whereas avoidant coping was negatively related with total SWL (r = 0.798, P < 0.01; r = −0.82, P < 0.01). The negative correlation is due to high levels of perceived stress scores resulting in lower levels of life satisfaction. There was no significant correlation between the emotion-focused coping strategies of patients and the total SWL.
Total TSWL was best predicted by a set of two coping strategies, namely problem focused and emotion focused (P < 0.05) as shown in Table 4. These two predictors together explained 73% variance in the criterion variable. Religious coping strategy was related positively, followed by active and adaptive coping strategies which were related negatively. Active coping strategy had explained 12.5% variance, planning explained 5.1%, and restraint coping explained 3.3% variance.

It was found that in two patient groups, namely cancer and HIV patients, judgment of satisfaction in life was predicted by the more use of active coping strategies. Only in the patients afflicted with HIV, adaptive coping strategies predicted SWL.
In both group of palliative patients, active coping strategies and acceptance were beneficial in terms of QOL, unlike avoidant coping strategies and venting of emotions.
Folkman and Lazarus believed that the skills people need to accommodate and to cope with stressful situations are often learned through experience.[1314] Those who have learned to use more emotion-focused coping responses to deal with stressful situations may be more depressed because of the ineffectiveness of that type of coping response. If problem-focused coping is more effective, individuals could be taught to use more problem-focused coping; such training might help them feel as if they had more control over the course of the illness.[181920]
Strengths of the study
-
Adequate sample size had been studied
-
Since there was only one examiner to interview the patients, the data collection procedure was uniform, thereby reducing interobserver bias
-
The results could bring out coping strategies which are associated with better SWL and that may be utilized in clinical practice.
Limitations of the study
-
This study suffers from limitations similar to those of any other cross-sectional study, such as lack of temporality for determining causal associations and no calculation of incidence and risk ratios for various outcomes
-
Findings of the study can only be extrapolated to hospitalized patients
-
Recall bias might be present
-
The participants in this study were already seeking support and may differ significantly from those who do not seek outside help.
Recommendations
-
Mental health professionals need to be aware of the various coping strategies that patients use to confront the diagnosis of their illness and its outcome. An assessment of coping strategies is a prerequisite to facilitate appropriate care for patients
-
Mental health professionals can assist the patients by providing support, information, and alternative strategies to promote coping strategies. They should consider appropriate intervention to help patients select appropriate coping strategies with them
-
Emotional and religious coping was the most common coping strategy used by the patients. Emotional support and spiritual support should be provided
-
Establishing support groups and involving their family to provide emotional support to the patients would be to the benefit of patients in the Indian context
-
Coping strategies such as behavioral disengagement, the venting, planning, and self-blame are all related to emotional distress
-
Mental health professionals can help patients to avoid strategies that induce emotional distress. They can do this by identify coping strategies, sharing information, exchanging ideas, and empowering them to use appropriated coping strategies to reduce emotional distress.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- Learned helplessness in humans: Critique and reformulation. J Abnorm Psychol. 1978;87:49-74.
- [Google Scholar]
- Quality of life in advanced cancer patients: The impact of sociodemographic and medical characteristics. British Journal of Cancer. 2001;85:1478-85.
- [Google Scholar]
- Dying young, dying poor: A sociological examination of existential suffering among low-socioeconomic status patients. J Palliat Med. 2004;7:27-37.
- [Google Scholar]
- Palliative Care for Older People: Better Practices 2011
- Anxiety, depression and coping strategies in breast cancer patients on chemotherapy. Malays J Psychiatry. 2010;19:19-24.
- [Google Scholar]
- Coping Strategies and Emotional Distress of Patients with Early Stage Breast Cancer and Their Spouses 2009
- Coping and emotional distress in primary and recurrent breast cancer patients. J Clin Psychol Med Settings. 2002;9:245-51.
- [Google Scholar]
- Coping strategies and life satisfaction: Chronically ill patients perspectives. J Indian Acad Appl Psychol. 2007;33:161-8.
- [Google Scholar]
- The relationship between coping and emotion: Implications for theory and research. Soc Sci Med. 1988;26:309-17.
- [Google Scholar]
- Appraisal, coping, health status, and psychological symptoms. J Pers Soc Psychol. 1986;50:571-9.
- [Google Scholar]
- Appraisals and coping in people living with cancer: A meta-analysis. Psychooncology. 2006;15:1027-37.
- [Google Scholar]
- Assessing coping strategies: A theoretically based approach. J Pers Soc Psychol. 1989;56:267-83.
- [Google Scholar]
- Stressors and coping strategies among female cancer survivors after treatments. Cancer Nurs. 2007;30:101-11.
- [Google Scholar]
- The relationship between life satisfaction and psychosocial variables: New perspectives. Subjective Well-Being: An Interdisciplinary Perspective 1991:141-69.
- [Google Scholar]
- Psycho-spiritual well-being in patients with advanced cancer: An integrative review of the literature. J Adv Nurs. 2003;44:69-80.
- [Google Scholar]






